

By Brian Harper, W-EMT, DMT
TRAVEL HEALTH | Nov 19, 2015
Consider the following scenario: You and your family are enjoyed an impromptu swim in a protected cove. After the early morning dip, you notice your young niece whose lips look slightly blue. She is huddled in a towel and still wearing a rash guard over her swimsuit. A breeze has picked up, and her hair is wet. You ask her if she's warm enough, and she just shrugs her shoulders. You mention that she might be warmer if she changes out of her wet items. "Yeah, I tried," she mumbles, "but I couldn't get them over my head."
Mild hypothermia is marked by shivering and a group of symptoms that can collectively be referred to as "the umbles." These include fumbling, mumbling and grumbling, which characterize a combination of lethargy, apathy and a decline in motor function. Fine motor skills are the first to go, and tasks like zipping up a jacket or tying shoes become difficult. The patient may neglect to take steps to minimize further heat loss, such as removing a wet swimsuit. Although it's often thought of as a cold water boating risk, hypothermia is particularly problematic at sea, even in warm weather, because of the way it can subtly steal one's ability to think clearly and make good decisions.

Join thousands of members who rely on DAN Boater's Medical Information Line for non-emergency medical assistance before, during and after travel.
To successfully prevent or treat hypothermia, attention should be given to each of the four mechanisms of heat transfer:

In addition to managing heat loss, it is a good idea to promote heat generation. Encourage the patient to eat and, if she is able, perform light exercise. Sweet foods in particular offer calories the body can use quickly. Out of concern for maintaining an airway, give a patient food only if she is able to eat it without assistance.
If cold stress becomes hypothermia and is not addressed in the early stages, the patient will begin to experience uncontrollable shivering and a decline in gross motor skills. These are signs that moderate hypothermia has begun. The patient's coordination will be impaired, ultimately manifesting as stumbling or an inability to walk. At this point, the need for intervention is critical. It may still be possible to rewarm this patient in the field; efforts should begin in earnest.
A patient with severe hypothermia will have lost the ability to shiver. Many basic body functions will slow down due to diminished core temperature. This patient may be unresponsive, and the heart rate may not be palpable. Respirations may be slow and faint. The objective of care should be to prevent further heat loss. Wrap the patient in as many insulating layers as are available, and use a tarp or tent fly to ensure that the patient and the insulating layers remain dry. Initiate an evacuation immediately, but take care to handle the patient gently. Violent movement could send the patient's heart into a potentially fatal rhythm. This combined with the possible difficulty identifying a heartbeat means that great care must be taken when assessing signs of life in severely hypothermic people. Chest compressions are appropriate only when signs of life are truly absent. Rescue breaths can be given freely, if needed.
MORE FROM
SAFE PASSAGE

TRAVEL HEALTH | Nov 19, 2015
Field Management of Hyperthermia
TRAVEL HEALTH | Oct 1, 2015
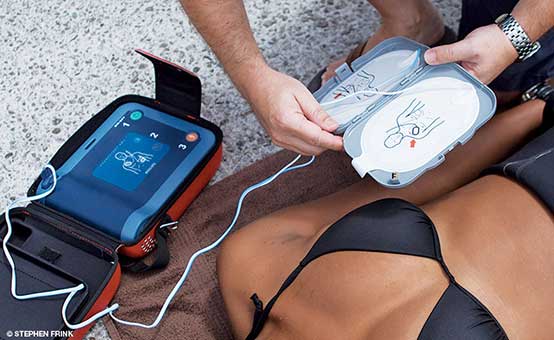
Are AEDs Safe To Use In Wet Environments?
THIS WEBSITE DOES NOT PROVIDE MEDICAL OR DENTAL ADVICE.
It is intended for general informational purposes only and does not address individual circumstances. It is not a substitute for professional medical or dental advice, diagnosis or treatment and should not be relied on to make decisions about your health. Never ignore professional medical or dental advice in seeking treatment because of something you have read on the DAN Boater website. If you think you may have a medical emergency, immediately call your doctor, dial 911, or contact emergency services nearest you.